Can Coughing Damage Your Vocal Cords? Causes, Symptoms, and Recovery
A cough protects your airway, but the same force that clears irritants from your lungs can quietly damage your vocal folds, the small bands of tissue in your throat that come together to create your voice. Each forceful cough slams them together, at about ten times the pressure of normal speech. Do that 14 or more times a day for weeks or months, and the strain can build up over time.
Chronic coughing is one of the most underrecognized causes of voice problems in adults, and the damage often goes unaddressed because adults assume hoarseness will resolve on its own.
Below, we cover how coughing damages the vocal cords, which symptoms signal a problem, which conditions drive chronic cough, and which treatment options, including voice therapy, can get your voice back on track.
Key Takeaways
Chronic cough strains the vocal cords: Repeated forceful coughing episodes inflame and stiffen the vocal folds, leading to symptoms such as hoarseness, vocal fatigue, and throat irritation that can persist long after the original illness clears.
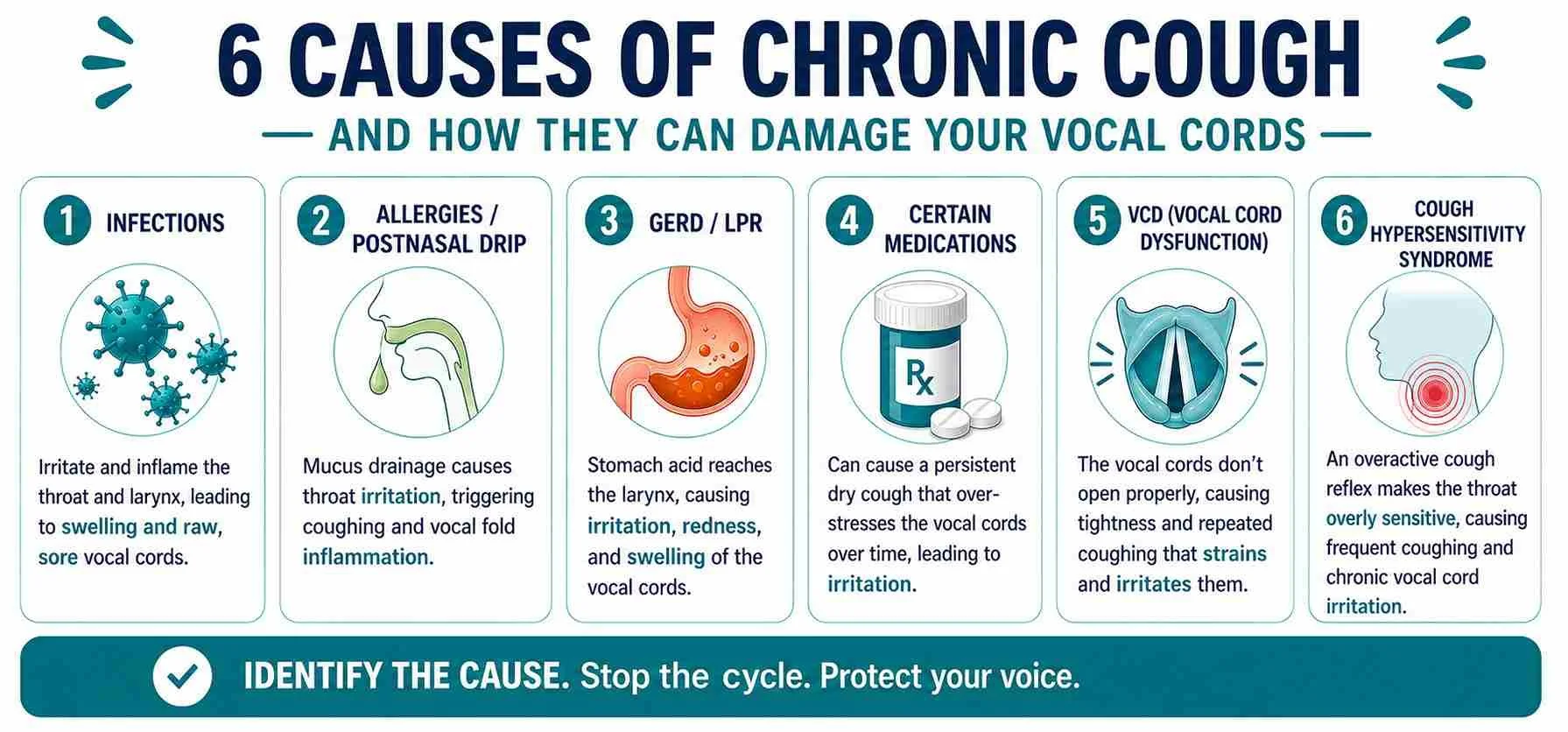
Common causes include allergies, GERD, LPR, infections, VCD, and certain medications: Identifying the root cause is essential; different triggers require different treatments to reduce irritation and stop the cycle.
A cough lasting more than eight weeks is chronic: At that point, vocal cord damage is more likely, and evaluation by an otolaryngologist (ENT) and speech-language pathologist is recommended.
Voice therapy and home strategies help: Speech-language pathologists use cough suppression techniques, breathing retraining, and vocal hygiene education to protect and rehabilitate the voice.
How Coughing Damages the Vocal Cords
What Are the Signs Your Vocal Cords May Be Damaged?
Does Vocal Cord Dysfunction Cause Chronic Cough?
How Are Vocal Cord Damage and Chronic Cough Diagnosed?
What Are the Treatment Options for Cough-Related Vocal Cord Damage?
How Can Adults Protect Their Voice While Still Coughing?
What We See Working with Adults
Frequently Asked Questions About Vocal Cord Damage from Coughing
How Coughing Damages the Vocal Cords
Your vocal folds sit inside the larynx (voice box), where two muscular bands of tissue open during breathing and close to produce sound, protect the airway, and support swallowing. During a cough, the folds seal shut, and air pressure in the lungs builds rapidly before being released in a powerful burst. That forceful expulsion clears the airway and also traumatizes the folds.
A single cough rarely causes lasting damage. The problem is repetition. Mild irritation from two weeks of coughing can resolve without treatment; irritation from two or more months of coughing episodes often cannot. The repeated trauma inflames and thickens the fold tissue, disrupts the smooth vibratory pattern needed for clear sound, and can trigger a hypersensitivity response in the laryngeal nerve network.
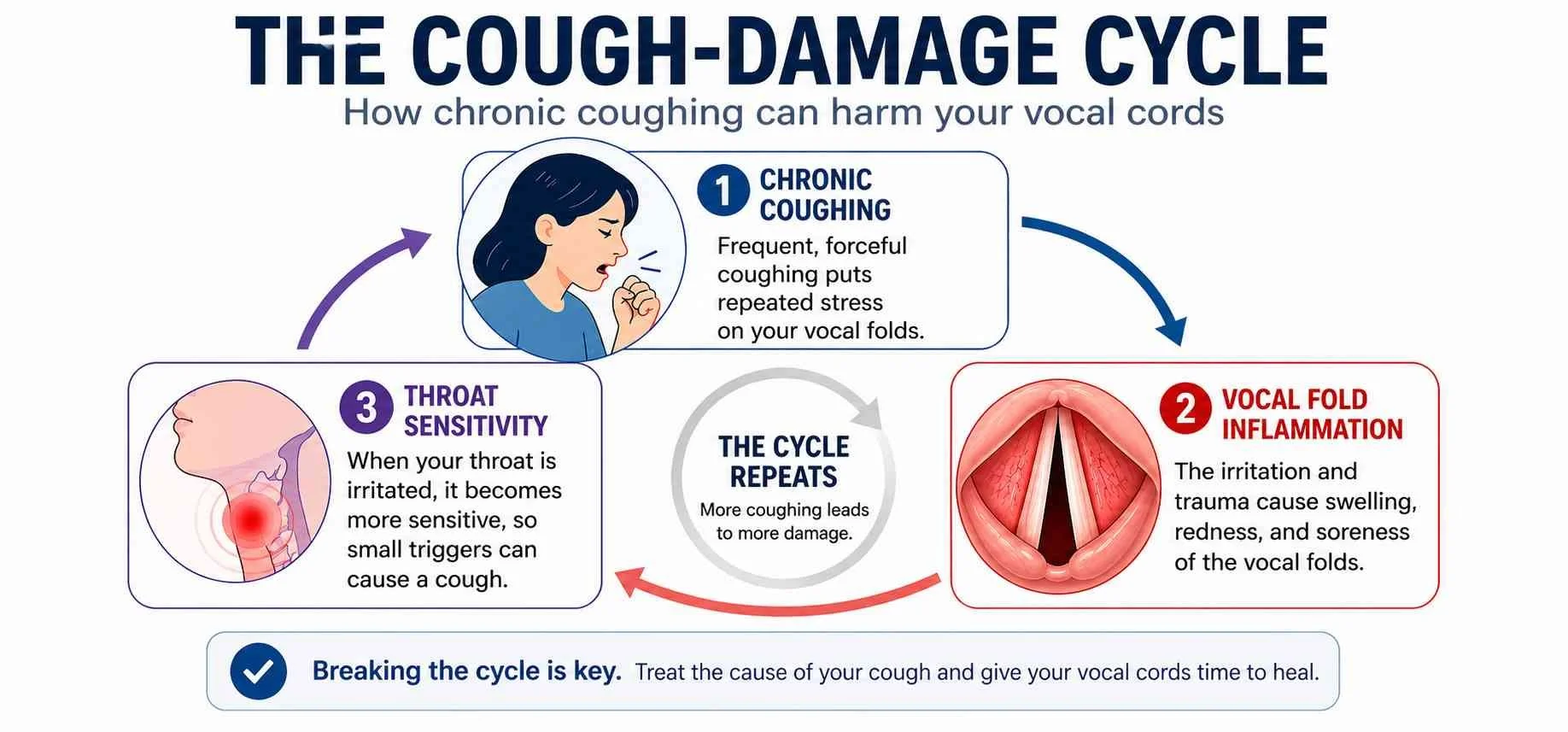
What makes chronic cough especially damaging is the cough-habit loop. Once the throat becomes sensitized after an illness, for example, and the brain continues to interpret minor residual irritation as a threat and sends a signal to cough even when the original cause has resolved.
The coughing then exacerbates the irritation, which leads to more coughing. Adults trapped in this cycle often don't realize the original illness is gone and the cough itself is now the problem.
Voice Therapy For Hoarseness: Learn How To Fix a Hoarse Voice
Check out our blog on voice therapy for hoarseness for more information!
What Are the Signs Your Vocal Cords May Be Damaged?
Vocal cord damage from coughing rarely arrives all at once. Symptoms build gradually, and many adults dismiss early warning signs as part of the illness that caused the cough.
Hoarseness is the most common indicator. When swelling thickens or stiffens the vocal folds, they can't vibrate smoothly, producing a rough, raspy quality. A tired voice often follows, and the voice drops in volume or clarity after only brief periods of talking or singing.
Beyond those primary symptoms, additional signs include breathiness (incomplete closure of the folds), throat pain during or after coughing, a sensation of a lump or tightness in the throat, and progressive changes in pitch or voice quality. In more severe cases, complete loss of voice can occur. Adults who experience hoarseness lasting more than two weeks should see a doctor, particularly if the cough is also persistent.
Symptoms range in severity depending on how long the cough has lasted and what is driving it. Mild irritation from a short illness may clear within days. Chronic coughing from asthma, gastroesophageal reflux disease (GERD), or vocal cord dysfunction can cause symptoms that persist for months without targeted treatment.
What Causes Chronic Cough?
A cough lasting fewer than three weeks is usually tied to an acute illness. One lasting three to eight weeks is subacute, and one persisting beyond eight weeks meets the clinical definition of chronic cough. At that duration, the likelihood of vocal cord involvement increases considerably.
Multiple conditions can drive chronic cough in adults. Understanding which one applies changes the treatment approach entirely.
Upper Respiratory Infections and Inflammation
Infections like colds or bacteria can irritate your throat and voice box, which can trigger a cough that lasts even after you feel better. Some bacterial infections may require antibiotics, while coughs after a virus can linger because the throat stays extra sensitive. Cutting down on irritants like smoke, dust, and strong fumes, and avoiding things like shouting or frequent throat clearing, can help your throat heal.
Allergies and Postnasal Drip
Allergies and sinus issues can cause postnasal drip, where excess mucus runs down the back of your throat and makes you cough or clear your throat frequently. Both of these can irritate your vocal folds, the small bands of tissue that help you produce your voice. Common triggers include pollen, dust, pet dander, and mold. Treating the allergy with antihistamines or nasal sprays can help reduce the mucus and the cough.
GERD and Laryngopharyngeal Reflux
Gastroesophageal reflux disease (GERD) causes stomach acid to flow back into the esophagus and, at times, reach the larynx. When it does, the result is laryngopharyngeal reflux (LPR), sometimes called silent reflux because it often occurs without heartburn.
Pepsin, a substance that comes up with stomach acid, can irritate your vocal cords. It can lead to ongoing irritation, swelling, and coughing, even if you don’t feel heartburn. Managing reflux with dietary changes, sleeping with your head elevated, and medications prescribed by a doctor can help reduce irritation.
Certain Medications
Some medications, including certain blood pressure drugs, can cause a persistent dry cough in some people. This happens because of the medication's effect on the airways. If you develop an ongoing, unexplained cough after starting a new medication, it’s worth talking with your doctor about whether a different option might work better without that side effect.
Cough Hypersensitivity Syndrome
Cough hypersensitivity syndrome (CHS) is a condition in which the laryngeal nerve becomes sensitized, triggering coughing in response to stimuli that would not bother most adults, including changes in air temperature, perfumes, talking, or even light touch on the throat. The threshold for cough activation is lowered far below normal.
Adults with CHS often describe their cough as constant or unpredictable, and standard cough treatments provide little relief. Management typically involves a speech-language pathologist working on cough suppression techniques combined with identifying and treating any underlying contributing conditions.
Does Vocal Cord Dysfunction Cause Chronic Cough?
Vocal cord dysfunction (VCD), also known as paradoxical vocal fold motion (PVFM), is a condition in which the vocal folds close during inhalation instead of opening. That closure restricts the airway and commonly produces a cough. Research by Vertigan et al. (2020) found that cough and VCD frequently co-occur: among adults presenting with chronic cough, 69 percent had moderate-to-severe PVFM on laryngoscopy. That overlap means adults with a persistent cough may have underlying VCD that hasn't been identified.
VCD is often confused with asthma because both produce breathing difficulties and a chronic cough. The key difference is that VCD-related airflow obstruction occurs during inhalation, while asthma involves expiratory obstruction. A flow-volume loop test and laryngoscopy can distinguish the two, though VCD is often triggered by the same irritants driving other chronic cough types, including postnasal drip, GERD, and airborne allergens.
How Are Vocal Cord Damage and Chronic Cough Diagnosed?
Diagnosing vocal cord damage from coughing requires input from two specialists: an otolaryngologist (ENT) and a speech-language pathologist. Each brings a different lens to the same problem.
The Role of the ENT
The ENT performs laryngoscopy, a procedure that uses a thin, flexible scope inserted through the nose or mouth to directly visualize the vocal folds. That visualization reveals inflammation, thickening, nodules, polyps, or lesions that formed from repeated coughing trauma. Stroboscopy adds a strobe-light component that allows the clinician to see subtle abnormalities in how the folds vibrate, identifying issues such as muscle weakness or early scar tissue formation.
The ENT may order tests like blood work to check for inflammation, breathing tests to look for asthma, or a simple test to see if stomach acid is coming up into your throat and causing irritation.
The Role of the Speech-Language Pathologist
Together, the ENT and speech-language pathologist coordinate care: the ENT addresses any medical or structural cause, and the speech-language pathologist leads the behavioral and functional recovery. In adults with VCD or cough hypersensitivity syndrome, the speech-language pathologist often serves as the primary treatment provider.
What Are the Treatment Options for Cough-Related Vocal Cord Damage?
Treatment depends on what is driving the cough and how much damage has already occurred. Most adults need a combination of approaches.
Voice Therapy
Cough suppression techniques teach adults to recognize cough triggers and interrupt the urge before it escalates, replacing forceful coughs with swallowing, gentle exhalation, or sipping water. Breathing retraining shifts breath support from the throat to the diaphragm, reducing laryngeal strain during both coughing and speaking.
Vocal hygiene education helps adults identify habits that worsen irritation, including excessive throat clearing, talking through fatigue, and whispering (which strains the folds more than normal speech). Research by Ryan et al. (2009) demonstrated that this type of behavioral treatment for chronic cough also improved paradoxical vocal fold motion and laryngeal hypersensitivity.
Medical Treatments
Depending on the cause, a doctor may recommend allergy medications or nasal sprays for postnasal drip, acid-reducing medications for reflux, antibiotics for certain infections, or inhalers to calm airway inflammation. If a medication you’re taking is causing a cough, your doctor may suggest switching to a different option.
Any medication should be discussed and monitored by your doctor, since the right choice and dose depend on your health history and other medications.
Home Strategies
Staying well hydrated keeps the vocal fold mucosa lubricated and reduces the friction that makes coughing more damaging. Using a humidifier in dry indoor environments, especially during the winter months, helps soothe the laryngeal tissue and reduce cough frequency.
Vocal rest means minimizing unnecessary talking and avoiding whispering, shouting, and singing until the folds have had time to recover. Avoiding smoke, dust, strong fumes, and known allergens reduces environmental irritants that perpetuate the cough cycle.
How Can Adults Protect Their Voice While Still Coughing?
Adults waiting for treatment to take effect, or managing a cough that can't be fully suppressed right away, can reduce vocal fold trauma with a few practical adjustments.
When you do need to cough, try to keep your lips slightly open or cough into a tissue to reduce the impact on your vocal folds. Taking a sip of water afterward can help soothe irritation. Speak at a comfortable volume and pace, and avoid pushing your voice when it feels tired.
Clearing your throat can be just as hard on your voice as coughing, and many people do it without noticing. Try replacing it with a swallow or a sip of water. Using steady, relaxed breathing and giving your voice short breaks during the day can also help reduce strain and prevent more irritation. Also, try to manage stress, which also compounds cough frequency and vocal fatigue.
What We See Working with Adults
Adults who come to us after months of coughing often describe the same experience: they've been told the illness is gone, but the cough stayed. By the time they reach us, many have tried multiple doctors and rounds of treatment without understanding why their voice still sounds rough and tired.
In sessions, we often see that the cough has become a habit, and the throat stays sensitive even after the original cause is gone. Adults often don't connect the constant throat clearing they do at work with the hoarse and tired voice they experience by evening. When we point out how frequently they're doing it and what it's costing the folds, it shifts the way they approach the problem.
The breakthrough usually comes not from eliminating the cough all at once, but from giving adults a replacement behavior. A hard swallow, a water sip, a moment of stillness.
Small changes can break the cycle without making it feel like you have to fight every urge. Voice quality often improves within a few weeks once the strain is reduced and the vocal folds have time to rest between sessions.
Frequently Asked Questions About Vocal Cord Damage from Coughing
1. What are the symptoms of vocal cord damage from coughing?
The most common symptoms are hoarseness, vocal fatigue, and a rough or raspy voice that persists beyond the acute illness. Adults often notice breathiness, throat tightness or soreness, reduced vocal range when singing, and difficulty projecting their voices. Symptoms that last longer than two weeks without improvement warrant evaluation by an ENT.
2. How long does it take for the vocal cords to heal after chronic coughing?
Mild irritation often improves within days to weeks once the cough is under control and you’re taking care of your voice. More significant issues, such as vocal fold lesions, ongoing sensitivity, or a cough that’s become a habit, can take a few months of targeted voice therapy to fully resolve. Starting early usually leads to a faster recovery.
3. Can coughing permanently damage vocal cords?
Most voice changes from coughing can improve with the right treatment. However, long-lasting or severe coughing can lead to issues like vocal fold nodules, polyps, scarring, or ongoing sensitivity that may take longer to manage. The risk of lasting changes increases when a chronic cough goes untreated for many months or years.
4. What is cough hypersensitivity syndrome, and how is it treated?
Cough hypersensitivity syndrome (CHS) happens when the nerves in your throat become overly sensitive, so even small triggers like changes in air temperature, talking, perfumes, or slight irritation can set off a cough. Treatment usually includes cough suppression and breathing techniques with a speech-language pathologist, as well as medical care for any underlying issues. Standard cough medications alone often aren’t enough to resolve it.
5. How does voice therapy help with vocal cord damage from coughing?
Voice therapy with a speech-language pathologist addresses the behavioral component of cough-related vocal cord damage. Voice therapy focuses on cough suppression strategies, breathing retraining, and vocal hygiene education to reduce ongoing trauma to the folds.
For adults with VCD or cough hypersensitivity syndrome, voice therapy is the primary treatment. Treatment for vocal cord dysfunction and cough-related voice issues is available through online sessions."
How Connected Speech Pathology Can Help
Connected Speech Pathology works with adults whose voices have been affected by chronic cough, vocal cord dysfunction, GERD, laryngeal hypersensitivity, and related conditions. Our speech-language pathologists provide the assessment and voice therapy entirely online, through secure video sessions that don't require travel or waiting room time.
We tailor each treatment plan to the specific cause and severity of the problem. For adults dealing with a habitual cough, we focus on cough suppression and behavioral retraining. Adults with VCD or laryngeal hypersensitivity benefit from specialized breathing and relaxation techniques that reduce episodes and improve airway control.
If you're dealing with hoarseness, vocal fatigue, or a cough that won't quit, a free consultation is the first step.
Summary
Chronic coughing damages the vocal cords through repeated forceful trauma that inflames, thickens, and sensitizes the fold tissue. Causes include upper respiratory infections, allergies, and postnasal drip, GERD, laryngopharyngeal reflux, certain medications, and vocal cord dysfunction.
Adults whose cough has lasted more than eight weeks, or whose voice hasn't returned to normal after a shorter illness, should seek evaluation from an ENT and a speech-language pathologist. Voice therapy addresses both the physical damage and the behavioral patterns that sustain it, with most adults seeing meaningful improvement within weeks of beginning treatment.
About the Author
Allison Geller is a communication coach, speech-language pathologist, and founder of Connected Speech Pathology, an international online practice providing professional communication coaching and speech therapy for children, teens, and adults. With more than two decades of experience, she has worked in medical and educational settings, published research on aphasia, and leads a team of specialists helping clients improve skills in public speaking, vocal presence, accent clarity, articulation, language, fluency, and interpersonal communication.